Patients With Limited English Proficiency: A Challenge for Oncology Nursing Providers
Background: Limited English proficiency (LEP) is a limited ability to read, write, speak, and understand English. About 145,000 individuals with LEP will be diagnosed with a new cancer annually, and English remains the dominant language spoken in the U.S. medical system.
Objectives: The goal of this article is to discuss the issues faced by patients with LEP and cancer who are unable to communicate effectively with oncology providers.
Methods: This overview used published U.S. government statistics, information from consensus and policy organizations, and clinical studies published between 2017 and 2022.
Findings: Federal laws prohibit discrimination based on immigration status. People with LEP experience delayed cancer diagnoses and often receive inadequate treatment. Patients with LEP often have limited understanding of the medical system and do not receive language-concordant information about their cancer and treatment options.
Jump to a section
Earn free contact hours: Click here to connect to the evaluation. Certified nurses can claim no more than 1 total ILNA point for this program. Up to 1 ILNA point may be applied to Nursing Practice OR Oncology Nursing Practice OR Professional Practice/Performance OR Psychosocial Dimensions of Care OR Quality of Life. See www.oncc.org for complete details on certification.
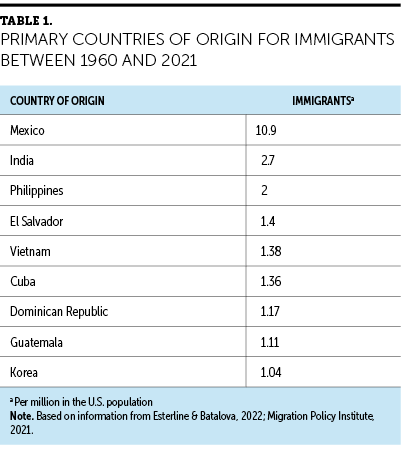
Limited English proficiency (LEP) is defined as English as a second language and a limited ability to read, write, speak, and understand the language (Foiles Sifuentes et al., 2020). Between 2016 and 2018, about 64 million Americans aged 5 years or older spoke a language other than English at home, of whom 40% reported that they speak English less than very well (Farina et al., 2022; U.S. Census Bureau, 2022). A 2022 report by the Migration Policy Institute reported that 25 million people, 8.2% of the U.S. population, have LEP (Esterline & Batalova, 2022). The United States’ immigrant population is expected to increase from 44.9 million in 2019 to 69 million by 2060 (Esterline & Batalova, 2022; Vespa et al., 2018), representing an increase from 13.5% to 17% of the total population (see Table 1). This is the second highest rate of immigration since 1890 when immigrants comprised 14.8% of the U.S. population (Esterline & Batalova, 2022). Asia has replaced Latin America as the main region from which U.S. immigrants originated (Vespa et al., 2018). The literature often uses the terms “foreign-born” and “immigrant” interchangeably when referring to people who were not U.S. citizens at birth, lawful permanent residents, refugee and asylum seekers, people on certain temporary visas, and unauthorized immigrants (Esterline & Batalova, 2022); this article will use “immigrant” as an all-inclusive term. Individuals born in the United States may also have LEP.
Cancer remains the second most common disease in the United States, with nearly 1.9 million new cancer cases expected in 2023 (American Cancer Society, 2023). Cancer care disparities among underrepresented and minority immigrant populations are increasing as population demographics continue to change (Alcaraz et al., 2019; Smith et al., 2009). Smith et al. (2009) predicted a 100% increase in cancer cases among underrepresented populations by 2030. Overall, cancer death rates have decreased in the United States, but immigrant populations still have a disproportionately higher incidence of cancer and mortality rates (Alcaraz et al., 2019). Fang and Ragin (2020) reviewed 42 studies pertaining to the topic and noted that immigrant, migrant, and refugee populations continue to experience a greater risk of cancer and have less access to cancer screening and health services. Although several studies have reported progress in reducing disparities in screening rates, it remains a challenge to close the gap in cancer screening among U.S. immigrants (Fang & Ragin, 2020).
It is estimated that about 145,000 people with LEP will be diagnosed with a new cancer annually (Farina et al., 2022). Although many people are emigrating from countries where English is not the predominant language (Vespa et al., 2018), English remains the dominant language spoken in the U.S. healthcare system.
The overarching goal of this article is to examine the healthcare issues posed by language barriers in the face of a growing immigrant population, recognizing that LEP is only one component of a complex set of social factors that affect health outcomes in immigrant populations with LEP. Oncology nurses and other healthcare providers (HCPs) are called upon to provide care to an increasingly diverse population. Oncology nurses provide direct patient care and serve as patient educators, cancer navigators, and leaders. Nurses play a critical role in advocating for patients with LEP. The American Nurses Association’s (2015) Code of Ethics for Nurses addresses individual actions and collective nursing intentions. The code of ethics requires each nurse to demonstrate ethical competence in the conduct of their professional life and to act courageously in protecting others and advocating on their behalf (American Nurses Association, 2015). The aims of this article are to (a) discuss the challenges for patients with LEP and cancer who are unable to communicate effectively with HCPs or within the healthcare system, (b) review the legal protections provided by the judicial system, and (c) describe the types of interpretation and translation services available for patients with LEP and associated barriers to effectively using these services.
Methods
This overview is based on data from the U.S. Census Bureau, U.S. Department of Health and Human Services (HHS), and U.S. Department of Justice; critically reviewed information from consensus and policy organizations; and synthesized relevant clinical studies pertaining to cancer care and health care in individuals with LEP that were published between 2017 and 2022.
Findings
Social Determinants of Health
Following the passage of the Patient Protection and Affordable Care Act (ACA), substantial efforts have been made to reform the U.S. healthcare system and to reduce disparities related to social determinants of health (HHS, 2023). Social determinants of health include language barriers, cultural differences, immigration status, neighborhoods, housing, education level, social conditions, access to health care, and economic constraints such as lack of health insurance coverage (Alcaraz et al., 2019). Cancer data collection does not typically include immigration variables, such as primary language spoken or country of origin (Alcaraz et al., 2019). However, the data that are available demonstrate considerable gaps in cancer screening and cancer care in immigrant individuals as compared to individuals born in the United States. Immigrants and individuals with LEP tend to live in communities where racial-, ethnic-, religion-, and nationality-based stigmas are prevalent (Alcaraz et al., 2019). There is a tendency for these individuals to avoid healthcare institutions for fear of discrimination, incarceration, and deportation, regardless of legal status (Alcaraz et al., 2019; Metchnikoff et al., 2018). These factors can delay the diagnosis of cancer and the start of treatments (Boscoe et al., 2016).
Effects of LEP on Issues Faced by Patients With Cancer
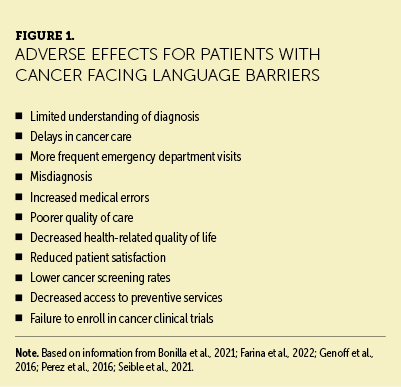
Studies have consistently identified adverse health effects in individuals with LEP (Al Shamsi et al., 2020; Foiles Sifuentes et al., 2020), particularly among Latin and Asian immigrants and other underrepresented ethnic populations in the United States. LEP is associated with poor comprehension in patient–provider interactions and trouble understanding medication labels (Al Shamsi et al., 2020). Individuals with LEP are at risk for healthcare disparities related to limited access to health care and not obtaining preventive services, such as cancer screening and early-detection screening (Foiles Sifuentes et al., 2020). A number of factors contribute to poor cancer outcomes, including the following: cultural and ethnic beliefs about cancer, inability to navigate the U.S. medical system, limited access to screening services, lack of health insurance, lack of language-concordant education about cancer and treatments, and institutional barriers impeding access to high-quality cancer care (Berdahl & Kirby, 2019; Perez et al., 2016) (see Figure 1). The diagnosis of cancer may be delayed in patients with LEP because they are less likely to have a regular HCP and often postpone visits because of apprehension or because they do not recognize symptoms of cancer. Individuals who live in poverty, whether they are immigrants or not, are diagnosed with later-stage cancers (Boscoe et al., 2016). Patients with LEP report difficulty expressing their symptoms to providers, which may lead to prolonged evaluations, incorrect diagnoses, delays in care, and extended hospital stays (Bonilla et al., 2021; de Moissac & Bowen, 2019; White et al., 2018). Perez et al. (2016) found that patients with LEP were given discharge paperwork and treatment instructions only in English. They often were not offered supportive services, such as visiting nurses and hospice care (Perez et al., 2016). Many patients reported not understanding their diagnosis or the prescribed treatment and therefore used an emergency department visit to clarify the diagnosis and proper medication dosing (de Moissac & Bowen, 2019; Diamond et al., 2019). Patients expressed a lack of confidence in the quality of care received and felt that their needs were unmet (de Moissac & Bowen, 2019; Seible et al., 2021). Discontented feelings with the healthcare system are correlated with feelings of distrust that affect participation in cancer treatments and clinical cancer trials (Farina et al., 2022).

Legal Protections for Patients With LEP
The U.S. legal system prohibits discrimination based on race, color, or national origin under the Civil Rights Act of 1964 (U.S. Department of Justice, 2000). Title VI of the Civil Rights Act of 1964 mandates that interpretation services be provided to patients with LEP. HCPs receiving federal funds are required to provide equal access to care for patients with LEP (U.S. Department of Justice, 2000). The National Culturally and Linguistically Appropriate Services (CLAS) Standards were formulated to reduce disparities and to aid providers to implement culturally and linguistically appropriate services to all patients (HHS, 2023). Further protections and recommendations were introduced in the expanded ACA (HHS, 2023). The ACA recommends linguistically appropriate patient education documents and signage, and provides financial incentives to hospitals to accommodate patients with LEP by providing qualified interpreters (Burkle et al., 2017). Ad hoc interpreters and a reliance on family members to serve as interpreters are generally discouraged.
The Office of Inspector General (2010) found that only 64% of surveyed hospitals met CLAS Standards when providing language assistance services. There are also discrepancies between the legal requirements and actual practice because most providers consistently used only ad hoc interpreters for communication (Diamond et al., 2019) and frequently used only English when informing patients of their rights, rather than using patients’ preferred language. Perez et al. (2016) identified underusing professional interpretation services as the primary factor affecting quality patient care. Perez et al. (2016) found that reasons for underusing translation services also included patient factors, particularly a lack of awareness that interpretation services are free, privacy concerns, and familial barriers.
Types of Available Interpretation and Translation Services
The use of trained medical interpreters and translation services improves health care, patient outcomes, and satisfaction with HCPs (Diamond et al., 2019; Lor & Martinez, 2020).
Live interpreters: In-person interpreters are preferred by HCPs whenever possible. This is not always an option because of scheduling conflicts, availability of specific languages, and costs (Burkle et al., 2017; Fiedler et al., 2022). Effectively using live interpreters requires training them and setting goals because live interpreters may edit the discussion, omit vital information, or falsely reassure the patient. These issues may be avoided by briefing the interpreter before meeting the patient and discussing expectations.
Video remote interpreters: Video remote interpreters provide rapid access to many languages at any hour of the day while being cost effective (Kushalnagar et al., 2019). The primary drawbacks to video remote interpreters are technical difficulties, connectivity issues, limited regional dialects, and limited available devices in the clinical setting (Kushalnagar et al., 2019). There is also the sense that video interpreters are less personal compared to live interpreters (Feiring & Westdahl, 2020).
Telephone or audio interpreters: Telephone or audio interpreters are a helpful option for simple questioning. Many HCPs prefer not to rely solely on telephone interpreters, citing concerns about communication skills, excessive background noise, and a lack of visual aids (Fiedler et al., 2022).
Ad hoc interpreters: Ad hoc interpreters, such as family, are often used because of convenience and the interpreter’s insight into the patient’s medical history, symptoms, medications, and current therapies (see Figure 2). Many patients prefer to use a family member rather than a professional interpreter (Burkle et al., 2017). However, ad hoc interpreters lack specific training and clinical knowledge that may impede accurate translation (Fiedler et al., 2022). Emotional involvement and paternalism may result in the interpreter withholding certain information. It may also be awkward for a family member to be thrust into a semiprofessional role for their own relative.

Bilingual staff members are often used as ad hoc translators. This is a valuable service, and staff members should be supported in completing formal interpreter training and certification. Although convenient, bilingual staff members possess similar deficiencies as family ad hoc interpreters. Most notably, bilingual staff members may lack the training or the knowledge of clinical terminology to provide proper translations.
Translation applications: Translation applications are mobile device applications that are readily available for digital download. A study by Hwang et al. (2022) suggested that there is enthusiasm among patients to learn about and use this resource. Nurses had concerns about mistranslation because they could not always verify the accuracy of the text and felt that there could be errors in regional dialects (Hwang et al., 2022). In these instances, nurses felt that the process was tedious, requiring multiple translation attempts to convey the right message (Hwang et al., 2022). Many of these translation applications are not designed for the clinical setting. Studies recommend that translation applications should not be replacements for professional interpreters and advise caution when using them (Panayiotou et al., 2019, 2020).
Barriers to Effective Interpretation Services and Suggestions for Improvement
Providing medical interpretation services for patients with LEP and cancer is a significant responsibility. Interpreters must modify the discussion to allow for culturally sensitive dialogue. Interpreters may experience discomfort when asked to deliver bad news because they may lack the proper training, experience, and emotional support capacity required. Efforts can focus on addressing the drawbacks that hinder certified interpreter use.
Provider barriers: HCPs often find it more expedient to avoid using any interpretation services because of time constraints and heavy workloads. HCPs may believe that they have established rapport with the patient and that the patient’s questions were “easy” (Martin et al., 2022; White et al., 2018). There is a sense that the amount of effort required to use an interpreter is not worthwhile (Jaeger et al., 2019). In a mixed-methods study of language interpretation, nurses described a preference for in-person interpreters for patients being discharged with medical devices that required the patient or family to perform complicated tasks (Lee et al., 2018). In contrast, they noted that telephone interpreters worked well for simple discharge instructions (Lee et al., 2018).
When interpretation services are readily available, HCPs are less likely to use their own nonproficient non–English language skills or ad hoc interpreters when communicating with patients. By establishing goals with the interpreter before the patient interview, HCPs can set expectations, provide pertinent clinical background, and build rapport with the interpreter. During the interview, short sentences are recommended to verify patient understanding while talking directly to the patient. It may be more effective for interpreters to translate the entire exchange, even if there is a prolonged exchange between the patient and the HCP. Debriefing with the interpreter is recommended because they may have noted certain subtleties, barriers, and reservations during the interaction. Similarly, debriefing allows HCPs to appreciate the interpreter’s well-being, perspective, and translation issues.
Institutional barriers: HCPs often express that in-person interpreters are difficult to schedule (Jaeger et al., 2019). Providers may be uncertain about how to set up a face-to-face meeting (White et al., 2018). Burkle et al. (2017) reported that providing interpretation services to patients with LEP leads to procedural delays because the average arrival time of the interpreter is 19 minutes but can occasionally take as long as 100 minutes. Hospitals and healthcare organizations can help by providing adequate and regularly maintained translation equipment, addressing connectivity issues, ensuring technological proficiency, and providing budgetary funds (Feiring & Westdahl, 2020; Jacobs et al., 2018).
Patient barriers: Even when medical interpreters were used, patients reported not fully understanding the information presented and feeling unequipped to ask questions (Perez et al., 2016). Patients reported that they felt ill-prepared to participate in treatment decisions and cited this as a contributor to treatment nonadherence. Patient-centered strategies focus on empowering patients by providing visual aids that describe the roles of interpreters and how to obtain translation services (Perez et al., 2016). Nurses can also educate patients about the U.S. medical system, advising them of their right to ask questions and to inform HCPs about their experience with adverse symptoms (Perez et al., 2016).
Discussion
The diagnosis of cancer is life-changing and the magnitude of information that patients receive on cancer type, stage of disease, and decisions about treatment options can be daunting, even more so for patients with LEP (Perez et al., 2016). Caring for patients with LEP presents a challenge for oncology providers because of the complexity of communicating information accurately while providing care that is compassionate and culturally sensitive (Yeo et al., 2011). Education and training in linguistically and culturally competent care can help to diminish barriers (Perez et al., 2016). Effective education initiatives can include the following: (a) providing formal training about caring for diverse populations (Yeo et al., 2011), (b) educating about the different types of interpretation services and the importance of using a certified medical interpreter, (c) offering language courses, (d) developing one’s language skills, (e) assessing competency in interpretation services, (f) raising awareness of interpretation services, (g) ensuring accessibility, and (h) encouraging staff from diverse backgrounds to become certified and trained in medical interpretation (Jaeger et al., 2019; Jones et al., 2020; Martin et al., 2022).

Implications for Practice
Communication between patients with cancer and oncology nurses can be influenced by individual biases, personal cultural beliefs, stereotypes, and learned behaviors (Yeo et al., 2011). Nurses can take immediate action to lessen these barriers. By recognizing differing cultural familial roles, values, and preferences, nurses can prioritize and improve the clinical experience for patients (Perez et al., 2016). By being familiar with available medical interpretation services and other resources (see Figure 3), nurses can lessen gaps in communication. In clinical areas, it is crucial to verify that interpretation devices are functional and well maintained. Nurses can strive to learn another language, at a minimum mastering essential medical terminology, and potentially proceed to earn an interpreter certification.

Conclusion
Caring for patients with LEP and cancer presents a series of opportunities to improve patient outcomes. Oncology nurses, nurse practitioners, and other HCPs can have a significant impact in reducing the stigma felt by patients with LEP by improving the quality of patient–provider interactions in oncology settings. The effectiveness of language-concordant care is well documented in improving patient outcomes. Improvements can be made to provide linguistically appropriate and culturally competent cancer care to a changing U.S. population. These challenges require a holistic approach that includes providing adequate resources and staffing, easily accessible language translation and interpretation services, and education and training on cultural differences, as well as making changes in the hospital culture. Addressing these challenges can level the playing field and reduce LEP-related cancer care disparities.

About the Authors
Carl L. Trube, BSN, RN, is a staff nurse in the acute care center at the University of Texas MD Anderson Cancer Center in Houston; and Theresa P. Yeo, PhD, MPH, ACNP-BC, AOCNP®, FAANP, is a professor in the Jefferson College of Nursing, codirector of the Jefferson Pancreas Tumor Registry, and a nurse practitioner in the Department of Surgery, all at Thomas Jefferson University in Philadelphia, PA. The authors take full responsibility for this content. The authors were participants in the Clinical Journal of Oncology Nursing Writing Mentorship Program. The article has been reviewed by independent peer reviewers to ensure that it is objective and free from bias. Trube can be reached at carltrb@gmail.com, with copy to CJONEditor@ons.org. (Submitted November 2022. Accepted January 3, 2023.)
References
Alcaraz, K.I., Wiedt, T.L., Daniels, E.C., Yabroff, K.R., Guerra, C.E., & Wender, R.C. (2019). Understanding and addressing social determinants to advance cancer health equity in the United States: A blueprint for practice, research, and policy. CA: A Cancer Journal for Clinicians, 70(1),31–46. https://doi.org/10.3322/caac.21586
Al Shamsi, H., Almutairi, A.G., Al Mashrafi, S., & Al Kalbani, T. (2020). Implications of language barriers for healthcare: A systematic review. Oman Medical Journal, 35(2), e122.
American Cancer Society. (2023). Cancer facts and figures, 2023. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and…
American Nurses Association. (2015). Code of ethics for nurses with interpretive statements. https://www.nursingworld.org/practice-policy/nursing-excellence/ethics/…
Berdahl, T.A., & Kirby, J.B. (2019). Patient-provider communication disparities by limited English proficiency (LEP): Trends from the U.S. medical expenditure panel survey, 2006–2015. Journal of General Internal Medicine, 34(8), 1434–1440. https://doi.org/10.1007/s11606-018-4757-3
Bonilla, J., Escalera, C., Santoyo-Olsson, J., Samayoa, C., Ortiz, C., Stewart, A.L., & Nápoles, A.M. (2021). The importance of patient engagement to quality of breast cancer care and health-related quality of life: A cross-sectional study among Latina breast cancer survivors in rural and urban communities. BMC Women’s Health, 21(1), 59. https://doi.org/10.1186/s12905-021-01200-z
Boscoe, F.P., Henry, K.A., Sherman, R.L., & Johnson, C.J. (2016). The relationship between cancer incidence, stage and poverty in the United States. International Journal of Cancer, 139(3), 607–612. https://doi.org/10.1002/ijc.30087
Burkle, C.M., Anderson, K.A., Xiong, Y., Guerra, A.E., & Tschida-Reuter, D.A. (2017). Assessment of the efficiency of language interpreter services in a busy surgical and procedural practice. BMC Health Services Research, 17(1), 456. https://doi.org/10.1186/s12913-017-2425-7
de Moissac, D., & Bowen, S. (2019). Impact of language barriers on quality of care and patient safety for official language minority Francophones in Canada. Journal of Patient Experience, 6(1), 24–32. https://doi.org/10.1177/2374373518769008
Diamond, L., Izquierdo, K., Canfield, D., Matsoukas, K., & Gany, F. (2019). A systematic review of the impact of patient-physician non-English language concordance on quality of care and outcomes. Journal of General Internal Medicine, 34(8), 1591–1606. https://doi.org/10.1007/s11606-019-04847-5
Esterline, C., & Batalova, J. (March 17, 2022). Frequently requested statistics on immigrants and immigration in the United States. Migration Information Source. https://www.migrationpolicy.org/article/frequently-requested-statistics…
Fang, C.Y., & Ragin, C.C. (2020). Addressing disparities in cancer screening among U.S. immigrants: Progress and opportunities. Cancer Prevention Research, 13(3), 253–260. https://doi.org/10.1158/1940-6207.CAPR-19-0249
Farina, E.G., Rowell, J., Revette, A., Haakenstad, E.K., Cleveland, J.L.F., Allende, R., . . . McCleary, N.J. (2022). Barriers to electronic patient-reported outcome measurement among patients with cancer and limited English proficiency. JAMA Network Open, 5(7), e2223898. https://doi.org/10.1001/jamanetworkopen.2022.23898
Feiring, E., & Westdahl, S. (2020). Factors influencing the use of video interpretation compared to in-person interpretation in hospitals: A qualitative study. BMC Health Services Research, 20(1), 856. https://doi.org/10.1186/s12913-020-05720-6
Fiedler, J., Pruskil, S., Wiessner, C., Zimmermann, T., & Scherer, M. (2022). Remote interpreting in primary care settings: A feasibility trial in Germany. BMC Health Services Research, 22(1), 99. https://doi.org/10.1186/s12913-021-07372-6
Foiles Sifuentes, A.M., Cornejo, M.R., Li, N.C., Castaneda-Avila, M.A., Tjia, J., & Lapane, K.L. (2020). The role of limited English proficiency and access to health insurance and health care in the affordable care act era. Health Equity, 4(1), 509–517. https://doi.org/10.1089/heq.2020.0057
Genoff, M.C., Zaballa, A., Gany, F., Gonzalez, J., Ramirez, J., Jewell, S.T., & Diamond, L.C. (2016). Navigating language barriers: A systematic review of patient navigators’ impact on cancer screening for limited English proficient patients. Journal of General Internal Medicine, 31(4), 426–434. https://doi.org/10.1007/s11606-015-3572-3
Hwang, K., Williams, S., Zucchi, E., Chong, T.W.H., Mascitti-Meuter, M., LoGiudice, D., . . . Batchelor, F. (2022). Testing the use of translation apps to overcome everyday healthcare communication in Australian aged-care hospital wards—An exploratory study. Nursing Open, 9(1), 578–585. https://doi.org/10.1002/nop2.1099
Jacobs, B., Ryan, A.M., Henrichs, K.S., & Weiss, B.D. (2018). Medical interpreters in outpatient practice. Annals of Family Medicine, 16(1), 70–76. https://doi.org/10.1370/afm.2154
Jaeger, F.N., Pellaud, N., Laville, B., & Klauser, P. (2019). Barriers to and solutions for addressing insufficient professional interpreter use in primary healthcare. BMC Health Services Research, 19(1), 753. https://doi.org/10.1186/s12913-019-4628-6
Jones, J., Rice, K., Cueto, V., Mojica, C.D.V., Stawitcke, M., Salem, S., . . . Blankenburg, R. (2020). Increasing health care workers’ proficiency with using professional medical interpretation: A workshop. MedEdPORTAL, 16, 11017. https://doi.org/10.15766/mep_2374-8265.11017
Kushalnagar, P., Paludneviciene, R., & Kushalnagar, R. (2019). Video remote interpreting technology in health care: Cross-sectional study of deaf patients’ experiences. JMIR Rehabilitation and Assistive Technologies, 6(1), e13233. https://doi.org/10.2196/13233
Lee, J.S., Nápoles, A., Mutha, S., Pérez-Stable, E.J., Gregorich, S.E., Livaudais-Toman, J., & Karliner, L.S. (2018). Hospital discharge preparedness for patients with limited English proficiency: A mixed methods study of bedside interpreter-phones. Patient Education and Counseling, 101(1), 25–32. https://doi.org/10.1016/j.pec.2017.07.026
Lor, M., & Martinez, G.A. (2020). Scoping review: Definitions and outcomes of patient-provider language concordance in healthcare. Patient Education and Counseling, 103(10), 1883–1901.
Martin, F.C., Philip, J., & McLachlan, S.-A. (2022). Healthcare professionals’ views of working with medical interpreters in a cancer setting: An exploratory study. Journal of Cancer Education, 37(4), 1115–1121. https://doi.org/10.1007/s13187-020-01927-7
Metchnikoff, C., Naughton, G., & Periyakoil, V.S. (2018). End-of-life care for unauthorized immigrants in the U.S. Journal of Pain and Symptom Management, 55(5), 1400–1407. https://doi.org/10.1016/j.jpainsymman.2018.01.012
Migration Policy Institute. (2021). Largest U.S. immigrant groups over time, 1960-present. https://www.migrationpolicy.org/programs/data-hub/charts/largest-immigr…
Office of Inspector General. (2010). Guidance and standards on language access services: Medicare providers. U.S. Department of Health and Human Services. https://oig.hhs.gov/oei/reports/oei-05-10-00050.pdf
Panayiotou, A., Gardner, A., Williams, S., Zucchi, E., Mascitti-Meuter, M., Goh, A.M., . . . Batchelor, F. (2019). Language translation apps in health care settings: Expert opinion. JMIR mHealth and uHealth, 7(4), e11316. https://doi.org/10.2196/11316
Panayiotou, A., Hwang, K., Williams, S., Chong, T.W.H., LoGiudice, D., Haralambous, B., . . . Batchelor, F. (2020). The perceptions of translation apps for everyday health care in healthcare workers and older people: A multi-method study. Journal of Clinical Nursing, 29(17–18), 3516–3526. https://doi.org/10.1111/jocn.15390
Perez, G.K., Mutchler, J., Yang, M.S., Tree-Mcgrath, C.F., & Park, E.R. (2016). Promoting quality care in patients with cancer with limited English proficiency: Perspectives of medical interpreters. Psycho-Oncology, 25(10), 1241–1245. https://doi.org/10.1002/pon.4176
Seible, D.M., Kundu, S., Azuara, A., Cherry, D.R., Arias, S., Nalawade, V.V., . . . Murphy, J.D. (2021). The influence of patient–provider language concordance in cancer care: Results of the Hispanic outcomes by language approach (HOLA) randomized trial. International Journal of Radiation Oncology, Biology, Physics, 111(4), 856–864. https://doi.org/10.1016/j.ijrobp.2021.05.122
Smith, B.D., Smith, G.L., Hurria, A., Hortobagyi, G.N., & Buchholz, T.A. (2009). Future of cancer incidence in the United States: Burdens on an aging, changing nation. Journal of Clinical Oncology, 27(17), 2758–2765. https://doi.org/10.1200/jco.2008.20.8983
U.S. Census Bureau. (2022). QuickFacts: United States. U.S. Department of Commerce. https://www.census.gov/quickfacts/fact/table/US/POP815220#POP815220
U.S. Department of Health and Human Services. (2023). Section 1557 of the Patient Protection and Affordable Care Act. https://www.hhs.gov/civil-rights/for-individuals/section-1557/index.html
U.S. Department of Justice. (2000). Enforcement of Title VI of the Civil Rights Act of 1964—National origin discrimination against persons with limited English proficiency; policy guidance. Office of the Federal Register. https://www.federalregister.gov/documents/2000/08/16/00-20867/enforceme…
Vespa, J., Medina, L., & Armstrong, D.M. (2018). Demographic turning points for the United States: Population projections for 2020 to 2060. U.S. Census Bureau. https://www.census.gov/content/dam/Census/library/publications/2020/dem…
White, J., Plompen, T., Osadnik, C., Tao, L., Micallef, E., & Haines, T. (2018). The experience of interpreter access and language discordant clinical encounters in Australian health care: A mixed methods exploration. International Journal for Equity in Health, 17(1), 151. https://doi.org/10.1186/s12939-018-0865-2
Yeo, T.P., Phillips, J., Delengowski, A., Griffiths, M., & Purnell, L. (2011). Oncology nursing: Educating advanced practice nurses to provide culturally competent care. Journal of Professional Nursing, 27(4), 245–254. https://doi.org/10.1016/j.profnurs.2011.03.004

